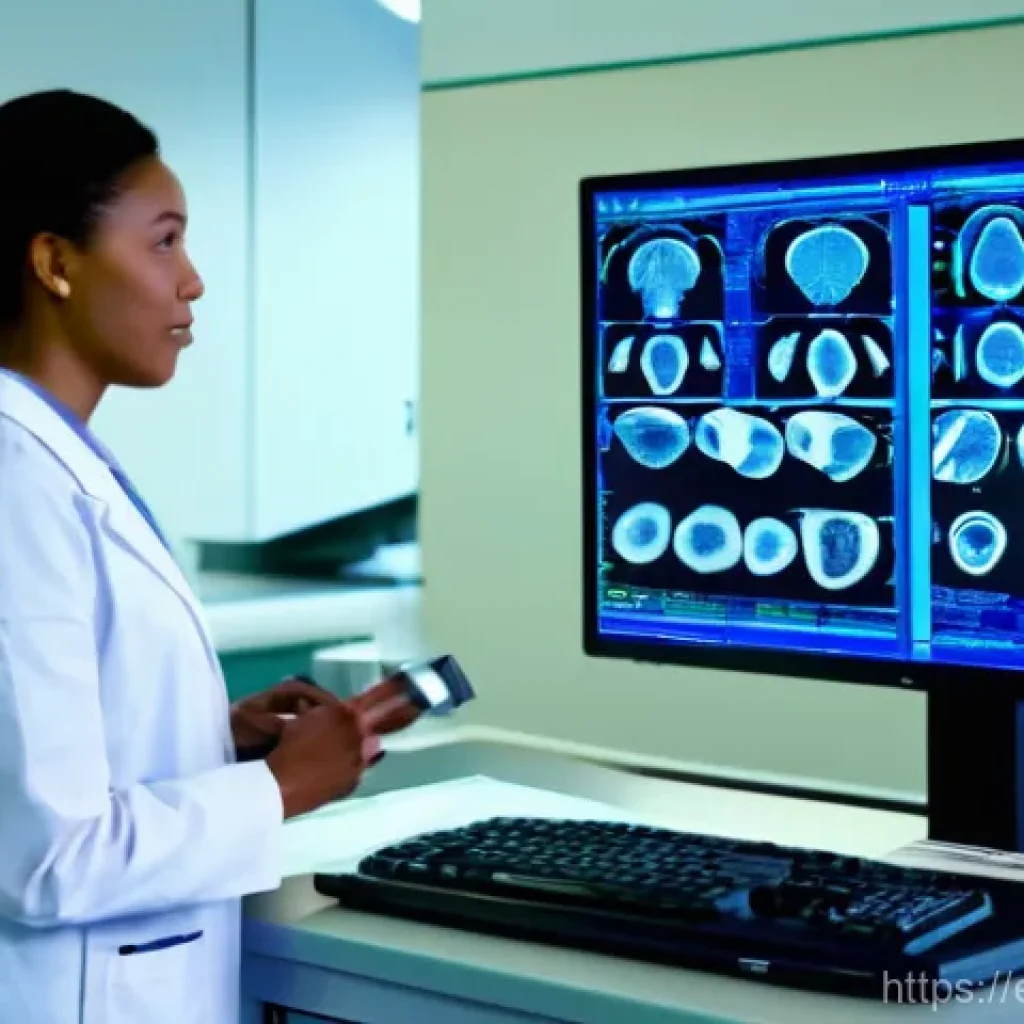
Hey there, healthcare enthusiasts and curious minds! Ever paused to think about the unsung heroes who work tirelessly behind the scenes to ensure you get the best medical care?
We often focus on doctors and nurses, and rightly so, but there’s a powerful, evolving partnership that’s absolutely vital: the collaboration between medical technologists and radiographers.
From my own observations within the medical community, I’ve seen firsthand how a truly seamless working relationship between these two critical professions can literally transform patient care, leading to faster, more accurate diagnoses and ultimately, better health outcomes.
It’s not just about running tests or taking scans anymore; it’s about a synchronized dance where every step matters, especially with technology moving at warp speed.
In today’s fast-paced medical landscape, where precision and efficiency are paramount, the synergy between clinical laboratory scientists and radiologic technologists is becoming more critical than ever before.
We’re talking about a future where AI-powered diagnostics in imaging merge effortlessly with lab results, creating a holistic view of patient health that was once unimaginable.
This isn’t just a trend; it’s the bedrock of modern, patient-centric care, driving advancements from early disease detection to personalized treatment plans.
Effective communication and interdisciplinary teamwork are breaking down traditional silos, reducing diagnostic errors, and speeding up turnaround times, which means quicker answers and peace of mind for patients.
It’s an exciting time to witness how these dedicated professionals are not only adapting but thriving in a technologically advanced environment, constantly innovating to deliver unparalleled care.
Want to understand how this incredible collaboration shapes your healthcare journey? Let’s uncover the essential insights together!
Beyond the Beakers and Scanners: A Unified Vision
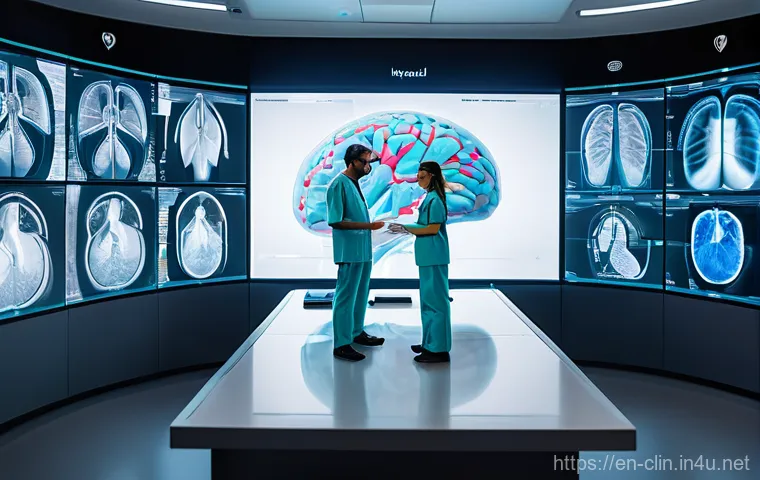
When I first stepped into the healthcare world, like many, I probably pictured labs as one thing and radiology suites as another entirely. But after years of observing the intricate dance that happens daily, it’s become profoundly clear to me that these two realms are far from separate islands.
What I’ve seen, time and again, is a beautiful convergence where the detailed findings from a clinical lab tech’s meticulous analysis perfectly complement the visual evidence captured by a radiographer.
It’s not just about one confirming the other; it’s about creating a richer, more comprehensive picture of a patient’s health that neither could achieve alone.
Imagine trying to solve a complex puzzle with half the pieces missing – that’s what healthcare would be without this powerful collaboration. It truly brings to life the adage that the whole is greater than the sum of its parts, offering patients a diagnostic clarity that would be impossible otherwise.
This shared vision ensures that every piece of information, whether microscopic or macroscopic, contributes to a robust understanding of the patient’s condition, ultimately paving the way for more targeted and effective treatment strategies.
From my personal experience in discussing cases with professionals in both fields, the respect and understanding for each other’s specialized input are palpable, driving a collective ambition to deliver exceptional care.
Connecting the Dots for Comprehensive Care
In our increasingly specialized medical world, it’s easy for disciplines to become siloed, but I’ve always advocated for breaking down those barriers, especially when it comes to diagnostics.
Clinical laboratory scientists, with their incredible precision in analyzing blood, tissue, and fluid samples, provide the foundational biochemical and cellular story of what’s happening internally.
Simultaneously, radiographers use advanced imaging techniques like X-rays, MRIs, and CT scans to give us a visual blueprint of organs, bones, and tissues.
What happens when these two sets of crucial data are effectively “connected”? It’s like watching a high-definition movie rather than just reading a script.
For instance, a radiographer might identify a suspicious mass, but it’s the lab technologist’s pathology report that can definitively characterize it as malignant or benign, guiding the next steps.
Or, a lab result indicating inflammation might prompt a specific imaging study to pinpoint the exact location and extent of the issue. This isn’t just theory; I’ve personally seen cases where a subtle lab marker combined with a nuanced imaging finding led to an early diagnosis that might have been missed if these professionals weren’t actively communicating and integrating their findings.
It’s this active linking of insights that truly elevates patient care from good to exceptional, ensuring no stone is left unturned in the diagnostic process.
The Power of Shared Insights
There’s something incredibly powerful about professionals from different specialties coming together, sharing their unique perspectives and insights. It’s not just about passing off results; it’s about a dialogue, a collaborative problem-solving session that happens, often implicitly, every day in hospitals and clinics.
From my vantage point, observing these interactions, I’ve seen how a radiographer might notice an unexpected finding on a scan and then, armed with knowledge of a patient’s recent lab work, instantly understand its significance.
Conversely, a lab technologist, aware of a patient’s imaging history, can interpret a lab value with greater context, perhaps highlighting an acute change that correlates with a visible anomaly.
This dynamic exchange of information, often informal but incredibly effective, helps to build a holistic patient profile. It minimizes the chances of misinterpretation and maximizes the speed at which critical decisions can be made.
When everyone is on the same page, bringing their piece of the puzzle to the table, the diagnostic pathway becomes smoother, faster, and far more accurate.
It fosters a culture of mutual respect and continuous learning, ultimately creating a stronger safety net for patients who rely on their collective expertise.
Decoding Health: When Lab Meets Image
In the intricate world of medical diagnostics, where every detail matters, the point where laboratory results merge with imaging findings is a truly fascinating intersection.
It’s here that the abstract data points from blood tests and tissue analyses gain tangible form through the visual clarity of X-rays, MRIs, and CT scans.
From my own observations, this confluence is where the real magic happens, transforming raw information into actionable insights for clinicians. Without the precise measurements of a clinical lab technologist, an imaging study might reveal an abnormality, but lack the specific biological context to fully understand its nature or severity.
Think of it this way: a radiograph can show you a shadow on the lung, but it’s the lab report that might tell you if that shadow is inflammatory, infectious, or even cancerous.
The dance between these two fields is continuous; one often triggers the need for the other, and together, they paint a complete picture that significantly reduces diagnostic uncertainty.
It feels like a constant feedback loop, where each specialty refines and validates the other’s findings, ensuring that the patient benefits from the most accurate and comprehensive assessment possible.
This deep integration is what truly underpins modern diagnostic medicine, making it far more robust and reliable.
Unraveling Complex Diagnoses
I’ve personally witnessed how challenging it can be to diagnose certain complex conditions based on a single type of information. This is where the synthesis of lab and image data becomes absolutely indispensable.
Take, for instance, autoimmune diseases; a patient might present with non-specific symptoms, and an initial imaging study could show some inflammation.
However, it’s the specific antibody markers identified by a clinical lab technologist that truly help unravel the autoimmune nature of the condition. Conversely, in cases of suspected infections, lab tests might identify the pathogen, but imaging can show the extent of the infection, say, in a specific organ, guiding treatment directly.
My experience tells me that these challenging cases are often solved not by a single heroic effort, but by the combined, meticulous work of both a radiographer meticulously capturing nuanced visual information and a lab technologist expertly interpreting biochemical signals.
They provide different lenses through which to view the same underlying pathology, and when these lenses are aligned, even the most elusive diagnoses begin to emerge with clarity.
It’s a testament to the power of interdisciplinary thinking and the crucial role each professional plays in solving medical mysteries.
Streamlining the Patient’s Diagnostic Path
One of the most profound benefits I’ve seen from this strong collaboration is how it streamlines the patient’s journey through the diagnostic maze. We all know how stressful and anxiety-inducing it can be waiting for answers, and a disjointed diagnostic process only exacerbates that.
However, when clinical lab scientists and radiographers work hand-in-hand, communicating effectively, they significantly reduce unnecessary tests, repeat procedures, and protracted waiting times.
For example, if a patient undergoes an urgent CT scan for abdominal pain, and the radiographer notes a finding that strongly suggests a specific type of infection, they can immediately flag it, allowing the lab to prioritize relevant blood cultures or inflammatory markers.
This proactive approach means patients get faster, more targeted follow-up, often avoiding days of uncertainty or additional, less relevant tests. It’s a prime example of efficiency driven by intelligence and collaboration, directly impacting patient satisfaction and, more importantly, leading to quicker initiation of appropriate treatment.
From my perspective, this seamless flow of information isn’t just about speed; it’s about empathetic care, minimizing the emotional and physical burden on patients during an already vulnerable time.
Elevating Accuracy: Precision Through Partnership
Accuracy is the cornerstone of effective healthcare, isn’t it? As someone who’s spent a considerable amount of time around medical professionals, I can tell you that every technologist, whether in the lab or in radiology, strives for absolute precision.
But what truly amplifies this individual dedication to accuracy is the partnership between clinical lab scientists and radiographers. It’s not just about doing their job well; it’s about their work validating and complementing each other’s, creating a feedback loop that significantly reduces the margin for error.
I’ve often thought of it as having two highly skilled proofreaders reviewing a critical document; each brings a unique perspective, catching nuances the other might miss.
For example, a lab result indicating a particular anomaly might prompt a radiographer to perform a more focused scan, or to scrutinize a specific area with greater intensity.
Conversely, an imaging finding might lead a lab technologist to rerun a test or investigate a specific marker more deeply. This kind of collaborative vigilance means that rare conditions are more likely to be identified, and common ones are diagnosed with greater certainty.
The outcome? A much higher degree of diagnostic confidence for the treating physicians and, most importantly, more reliable answers for the patients.
Minimizing Errors, Maximizing Trust
Errors in healthcare are something everyone wants to avoid, and I’ve seen firsthand how the collaborative efforts of lab technologists and radiographers are crucial in minimizing them.
When these two disciplines align, they create a built-in system of checks and balances. For instance, if a lab result seems unexpectedly high or low, a quick review of recent imaging might reveal an anatomical anomaly or a procedural factor that explains the discrepancy, preventing a misinterpretation.
On the flip side, an unclear spot on an X-ray might gain clarity when paired with a specific biomarker from the lab, preventing unnecessary anxiety or invasive follow-up.
This cross-referencing and contextualization are incredibly powerful. It’s not just about reducing mistakes; it’s about building an unwavering foundation of trust in the diagnostic process.
Patients and clinicians alike can rest easier knowing that two distinct, highly specialized perspectives have converged to confirm a diagnosis. From my observations, the best healthcare facilities actively foster this kind of interdepartmental communication precisely because they understand its critical role in enhancing patient safety and diagnostic reliability.
It’s about collective responsibility leading to individual excellence.
The Synergy of Technology and Expertise
We live in an era where technology is constantly advancing, bringing incredible tools to both the lab and the radiology suite. However, it’s the human expertise that truly unlocks the potential of these machines, and the synergy between lab techs and radiographers magnifies this.
Clinical lab scientists now utilize automated analyzers and molecular diagnostics that can detect diseases at unprecedented levels of sensitivity, while radiographers operate sophisticated MRI machines and CT scanners that generate incredibly detailed 3D images.
But without the other, each might only tell half the story. I’ve seen how integrating advanced lab data, like genetic markers, with state-of-the-art imaging, such as functional MRI, can provide an almost unparalleled understanding of diseases like certain neurological disorders.
It’s not simply running tests or taking scans; it’s about interpreting complex data sets, identifying patterns, and then cross-referencing these findings using their combined, deep expertise.
This synergy ensures that the patient benefits from both the cutting edge of scientific instrumentation and the nuanced understanding of experienced professionals working in concert.
The result is a diagnostic process that is not only highly advanced but also deeply informed, providing a level of insight that truly makes a difference in patient outcomes.
The Patient Experience: A Seamless Journey
When we talk about healthcare, it’s easy to get caught up in the technical jargon and complex procedures. But at the heart of it all, for me, is the patient.
And from the patient’s perspective, a seamless journey through diagnosis and treatment is paramount. What I’ve seen is that the collaboration between medical technologists and radiographers plays a surprisingly significant role in achieving this seamlessness.
When these two teams are in sync, patients experience fewer delays, less confusion, and a greater sense of confidence in their care. Imagine being sick and having to explain your symptoms multiple times to different departments, or waiting days for results that should be integrated.
That’s a frustrating and often terrifying experience. However, when the lab and imaging departments are communicating effectively, sharing context and prioritizing based on each other’s findings, the patient often feels like they are moving through a well-oiled machine, rather than a bureaucratic maze.
This isn’t just about efficiency; it’s about empathy, making a daunting process feel as smooth and reassuring as possible. It truly transforms the patient’s journey from a series of disconnected events into a coordinated effort focused entirely on their well-being.
Faster Answers, Greater Peace of Mind
I can’t stress enough how much faster answers can impact a patient’s peace of mind. Waiting for diagnostic results is one of the most agonizing parts of any illness.
From what I’ve observed, when clinical lab scientists and radiographers collaborate efficiently, they dramatically shorten this waiting period. For example, if an emergency room patient comes in with symptoms suggesting a stroke, a radiographer can quickly perform a CT scan to look for brain hemorrhage, and simultaneously, the lab can run critical blood tests like coagulation panels.
If a clot is identified through imaging, and lab results confirm specific parameters, treatment, such as clot-busting medication, can be initiated almost immediately.
This rapid turnaround, born from coordinated effort, can be the difference between full recovery and significant disability. It’s not just in emergencies; for routine check-ups or chronic disease management, timely and integrated results allow for quicker adjustments to medication or treatment plans, reducing patient anxiety and improving outcomes.
For me, seeing a patient’s relief when they get clear, timely answers because departments worked together so effectively is one of the most rewarding aspects of observing modern healthcare.
Personalized Care, Built on Collaboration
In an age where personalized medicine is becoming the gold standard, the robust collaboration between medical technologists and radiographers is laying some truly essential groundwork.
I’ve realized that true personalized care isn’t just about tailoring a treatment; it’s about building a uniquely comprehensive diagnostic profile for each individual patient.
For example, knowing a patient’s specific genetic markers from the lab can guide a radiographer in how to best interpret certain imaging features, or even what specific imaging protocol might be most beneficial to reveal subtle nuances relevant to that genetic predisposition.
Conversely, if a particular anatomical variation is noted on an image, the lab might be alerted to watch for specific anomalies in blood or tissue samples.
This deep level of communication allows for diagnostic strategies that are incredibly precise and tailored to the individual, far beyond a generic “one-size-fits-all” approach.
My experience tells me that this level of integrated understanding transforms patient care from a standardized process into a truly bespoke journey, where every test and every image contributes to a perfectly chiseled understanding of that person’s unique health story.
It’s truly inspiring to see this level of dedication to individualized medicine.
| Aspect of Collaboration | Clinical Lab Scientist Contribution | Radiographer Contribution | Integrated Patient Benefit |
|---|---|---|---|
| Initial Diagnostic Clues | Identifies biochemical markers, cellular abnormalities (e.g., elevated cardiac enzymes, abnormal blood counts). | Visualizes anatomical changes, structural anomalies (e.g., fracture, tumor presence, organ enlargement). | Faster identification of potential health issues, guiding immediate next steps. |
| Confirming Diagnoses | Provides definitive pathological diagnosis (e.g., cancer staging, infectious agent identification). | Confirms location, size, and extent of disease or injury through precise imaging. | High-confidence diagnosis, reducing uncertainty and preventing misdiagnosis. |
| Treatment Monitoring | Tracks changes in disease markers, drug levels, or inflammatory responses over time. | Monitors changes in lesion size, healing progress, or fluid accumulation in response to therapy. | Allows for real-time adjustment of treatment plans, optimizing therapeutic outcomes. |
| Emergency Response | Rapidly provides critical values (e.g., blood type for transfusion, electrolyte balance). | Quickly identifies acute life-threatening conditions (e.g., internal bleeding, stroke). | Expedited, life-saving interventions based on immediate, complementary information. |
Navigating Tomorrow’s Medical Frontier
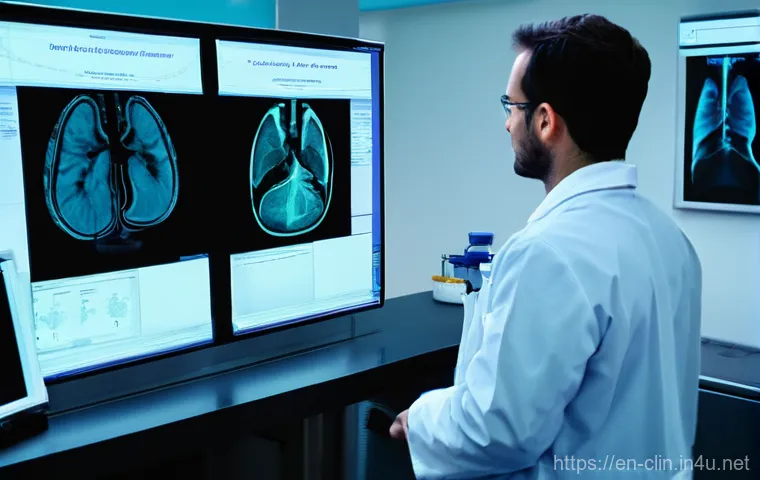
The medical world is in a constant state of evolution, and honestly, it’s thrilling to watch. What I’ve noticed is that the best healthcare professionals aren’t just keeping up; they’re actively shaping the future.
This is especially true for clinical lab scientists and radiographers, who are at the forefront of integrating cutting-edge technologies into daily practice.
The sheer volume of data generated by both the lab and imaging departments is immense, and learning how to harness it effectively is the next big challenge.
We’re talking about a future where AI isn’t just a buzzword but a practical tool that enhances their capabilities, not replaces them. From my perspective, this isn’t a threat; it’s an incredible opportunity for these teams to work even more closely, leveraging advanced analytics to unlock insights that were previously unimaginable.
They’re not just users of technology; they’re innovators, constantly pushing the boundaries of what’s possible in diagnostics. It feels like a pivotal moment, where their combined expertise will be instrumental in guiding how these new tools are safely and effectively implemented for the ultimate benefit of patients.
Embracing AI and Advanced Analytics Together
The whispers of AI in healthcare are growing into a roar, and I’ve been fascinated to see how both clinical lab scientists and radiographers are positioning themselves to embrace it.
For radiographers, AI is already proving invaluable in identifying subtle anomalies on scans that might be missed by the human eye, or in speeding up the analysis of large imaging datasets.
In the lab, AI algorithms are being developed to interpret complex genetic sequencing results or to flag unusual patterns in routine blood work, enhancing diagnostic speed and accuracy.
But here’s the crucial part: it’s not just about one discipline adopting AI. I’ve heard discussions about how AI-powered insights from imaging could directly inform the types of genetic tests prioritized in the lab, and vice-versa.
This kind of integrated AI approach, where algorithms are trained on combined lab and imaging data, holds the potential to create a truly holistic diagnostic engine.
It’s clear to me that these professionals, working in unison, will be the architects of these new AI-driven workflows, ensuring that technology serves to augment their human expertise, creating an even more powerful diagnostic force for patients.
Continuous Learning and Interdisciplinary Growth
One of the most admirable qualities I consistently observe in healthcare professionals is their commitment to continuous learning. This is particularly vital for clinical lab scientists and radiographers, given the rapid pace of technological advancements in both their fields.
It’s not enough to master one’s own domain anymore; there’s an increasing need for interdisciplinary growth. I’ve witnessed more and more training programs and professional development opportunities that bring these two groups together, not just to learn about each other’s roles, but to collaboratively explore new techniques and technologies.
For example, understanding the principles behind a novel molecular diagnostic test helps a radiographer better contextualize an imaging finding, and knowing how a new imaging modality works allows a lab technologist to better understand the clinical significance of their test results.
This cross-pollination of knowledge fosters a deeper mutual respect and, more importantly, equips them to tackle future challenges as a cohesive unit.
It feels like a shift from simply coexisting to actively co-evolving, preparing them to lead the charge in future medical innovations and patient care strategies.
Operational Excellence: Driving Efficiency in Healthcare
In any high-stakes environment, efficiency isn’t just a nice-to-have; it’s absolutely essential. And in healthcare, where patient outcomes often depend on speed and precision, operational excellence is a critical goal.
What I’ve observed over my years of interacting with medical teams is that the collaboration between clinical lab scientists and radiographers is a powerful, yet often unsung, driver of this efficiency.
When these two departments function like a well-oiled machine, the entire healthcare system benefits. We’re talking about reducing bottlenecks, minimizing redundant efforts, and ultimately, ensuring that resources are utilized optimally.
It’s not just about cutting costs, though that’s a positive side effect; it’s primarily about maximizing the delivery of timely, high-quality care. From my perspective, this isn’t achieved through mandates or top-down directives alone, but through the organic development of strong working relationships and clear communication channels between these crucial diagnostic teams.
Their shared commitment to the patient often translates directly into innovative solutions for improving workflow and accelerating diagnostic pathways.
Optimizing Workflows for Swift Outcomes
I’ve seen firsthand how a truly optimized workflow can transform the patient experience. When clinical lab scientists and radiographers communicate effectively, they can significantly streamline diagnostic processes.
Imagine a scenario where a stat lab test is needed to clear a patient for an urgent MRI. If the lab technologist and radiographer are in close contact, the lab can prioritize that specific test, and the imaging department can adjust their schedule to accommodate the patient as soon as results are available.
This prevents unnecessary waiting times and ensures that critical decisions can be made without delay. It’s about more than just individual tasks; it’s about understanding the entire patient journey and identifying where collaborative efforts can remove friction.
My experience tells me that when these teams routinely engage in cross-departmental huddles or utilize integrated information systems, they naturally identify ways to pre-empt delays and ensure a smoother, faster progression through diagnosis.
This not only benefits the patient with swift outcomes but also boosts the morale of the staff, who feel like part of a truly cohesive and effective team.
Resource Allocation: A Collaborative Approach
One aspect of operational excellence that often gets overlooked in the broader discussion is resource allocation, and here too, the collaboration between lab and imaging departments shines.
Healthcare resources, whether they are specialized equipment, skilled personnel, or even specific reagents, are precious. What I’ve observed is that when clinical lab scientists and radiographers work together, they can make more informed decisions about how to best utilize these resources.
For example, if a radiographer identifies a particular imaging finding that strongly points to a specific condition, the lab can then focus its more expensive or time-consuming tests on confirming that suspicion, rather than running a broad panel of less likely tests.
This intelligent prioritization, driven by shared diagnostic insights, ensures that resources are deployed where they will have the greatest impact. It avoids wasteful spending and ensures that specialized equipment and staff are available for the patients who need them most.
From my perspective, this collaborative approach to resource management isn’t just fiscally responsible; it’s a profound demonstration of their commitment to efficient, high-quality patient care across the entire facility.
The Human Element: Cultivating Stronger Teams
Beneath all the technology, the intricate procedures, and the scientific advancements, healthcare is fundamentally about people. And what truly makes a healthcare system thrive, from what I’ve observed, is the strength of its human teams.
The collaboration between clinical lab scientists and radiographers isn’t just about sharing data; it’s about building genuine relationships, fostering mutual understanding, and cultivating a shared sense of purpose.
When these professionals feel connected and valued, not just within their own departments but across the diagnostic spectrum, the entire working environment improves.
It creates a more supportive, less stressful atmosphere, which inevitably translates into better patient care. I’ve often seen how a simple friendly conversation or a quick huddle to discuss a tricky case can solidify these interdepartmental bonds, transforming colleagues into true collaborators.
It feels less like distinct silos and more like an integrated network of professionals, all pulling in the same direction for the patient’s benefit. This human element is, for me, the most beautiful and impactful part of their partnership.
Building Bridges Through Communication
Effective communication is the lifeblood of any successful team, and in the complex world of healthcare, it’s absolutely non-negotiable. I’ve learned that the most effective collaborations between clinical lab scientists and radiographers are built on strong communication channels, both formal and informal.
It’s not just about standardized reports; it’s about picking up the phone to discuss an unusual finding, sending a quick secure message to clarify a patient’s history, or even cross-departmental meetings to discuss challenging cases.
From my perspective, these seemingly small acts of communication build crucial bridges of understanding and trust. A radiographer might call the lab to ask about a specific blood marker related to an imaging finding, or a lab tech might reach out for details on a patient’s scan that could explain an atypical lab result.
This open dialogue prevents misinterpretations, speeds up problem-solving, and ensures that critical information isn’t lost in translation. It creates a dynamic where questions are encouraged, and clarification is always sought, leading to a much more robust and reliable diagnostic process for every single patient.
Recognizing Each Other’s Indispensable Roles
There’s a profound strength that comes from genuinely recognizing and appreciating the indispensable roles each team member plays. I’ve noticed that when clinical lab scientists truly understand the complexities of capturing high-quality images, and when radiographers grasp the meticulous detail involved in lab analysis, a deeper respect emerges.
This mutual appreciation is vital for fostering a cohesive working environment. It’s about acknowledging that neither can achieve the comprehensive diagnostic picture alone; they are truly interdependent.
This recognition helps break down any lingering departmental rivalries or misunderstandings, replacing them with a shared sense of purpose and collective pride in their joint contributions to patient care.
My experience shows that healthcare facilities that actively promote this kind of interdisciplinary appreciation often have higher staff satisfaction and, more importantly, deliver superior patient outcomes.
When everyone understands and values the critical piece of the puzzle that their colleagues provide, it elevates not just individual performance, but the entire diagnostic ecosystem to a truly exceptional level.
Wrapping Things Up
As we’ve explored together, the synergy between clinical lab scientists and radiographers isn’t just a nice idea; it’s the bedrock of modern, patient-centered healthcare. From my own journey observing these dedicated professionals, it’s clear that their collaborative spirit and integrated expertise are what truly transform raw data into a clear diagnostic picture. It’s a powerful testament to how teamwork, advanced technology, and unwavering dedication come together to ensure that each of us receives the most accurate and compassionate care possible. This partnership truly elevates the entire medical experience, offering peace of mind and better health outcomes for everyone.
Useful Insights for Your Health Journey
Here are some quick takeaways to help you navigate your own healthcare experiences:
1. Always Ask Questions: Don’t hesitate to ask your doctor or healthcare provider to explain your lab results or imaging reports in plain language. Understanding your health information is your right and helps you make informed decisions. Sometimes, misinterpreting results can lead to unnecessary anxiety, so a conversation with your provider is always best.
2. Keep Records: Maintain a personal file of your important medical documents, including past lab results and imaging reports. This can be incredibly helpful for new doctors or when seeking second opinions, providing a comprehensive historical view of your health.
3. Understand the “Why”: Before undergoing any test, ask why it’s being ordered and what specific information your healthcare team hopes to gain. This empowers you as a patient and clarifies the diagnostic pathway, ensuring you’re an active participant in your care.
4. Advocate for Integration: If you feel there’s a disconnect, gently inquire if your lab and imaging results are being viewed in conjunction. Many facilities actively work towards integrated diagnostics for improved accuracy and efficiency, but a polite question can ensure a holistic review of your case.
5. Utilize Patient Portals: Most modern healthcare systems offer online patient portals where you can access your results. Reviewing them can give you a head start on understanding your condition before your follow-up appointment, but remember to discuss them with your doctor before drawing conclusions.
Key Takeaways
In essence, the collaborative spirit between clinical lab scientists and radiographers is fundamental to accurate, efficient, and patient-centered diagnostics. Their combined expertise streamlines the healthcare journey, reduces diagnostic uncertainty, and ultimately leads to better, more personalized treatment outcomes. This partnership, bolstered by technology and continuous learning, is crucial for improving patient safety and elevating the standard of care for all of us.
Frequently Asked Questions (FAQ) 📖
Q: What exactly do medical technologists and radiographers do, and why is their collaboration so essential for accurate diagnoses?
A: Think of it this way: medical technologists, also known as clinical laboratory scientists, are the detectives of the microscopic world. They’re meticulously analyzing your blood, urine, tissue, and other body fluids using sophisticated equipment like microscopes and automated cell counters to uncover the tiniest clues about your health, like identifying infections, checking organ function, or even diagnosing conditions like cancer or diabetes.
They’re behind the scenes, yet their work informs about 70% of medical decisions. On the other side, radiographers, or radiologic technologists, are the masters of imaging.
They’re the ones using X-rays, CT scans, MRIs, and ultrasounds to capture detailed pictures of your internal anatomy, revealing injuries, tumors, or other abnormalities that aren’t visible from the outside.
Now, why is their teamwork so critical? Because often, neither a lab test nor an image tells the whole story on its own. It’s like having two pieces of a puzzle.
A medical technologist might find elevated inflammatory markers in your blood, but a radiographer’s scan might pinpoint the exact location and extent of the inflammation.
When these two professionals combine their expertise, sharing their findings and insights, they create a comprehensive, holistic view of your health. I’ve seen firsthand how this integrated approach minimizes diagnostic errors, accelerates the diagnostic process, and empowers doctors to make more precise and personalized treatment plans.
It’s truly where the magic happens for accurate and timely diagnoses!
Q: How does the synergy between medical technologists and radiographers directly benefit me as a patient?
A: That’s a fantastic question, and one that hits close to home for all of us! From a patient perspective, the collaboration between medical technologists and radiographers translates into several tangible benefits that enhance your entire healthcare journey.
First and foremost, you get faster, more accurate diagnoses. Instead of waiting days for different results to trickle in and be interpreted separately, an integrated approach means your lab data and imaging findings can be compared almost in real-time.
I’ve observed situations where this has shaved significant time off diagnosis, which can be critical for conditions like heart attacks or strokes where every minute counts.
Secondly, it leads to more personalized and effective treatment plans. When your care team has a complete picture—what’s happening at the cellular level from lab tests, and what’s visibly happening inside your body from scans—they can tailor treatments much more precisely to your unique condition.
This means less trial-and-error and more targeted interventions, which, in my experience, significantly improves outcomes and reduces unnecessary procedures.
Finally, and perhaps most importantly, this teamwork fosters enhanced patient safety and peace of mind. Better communication and reduced diagnostic errors mean fewer misinterpretations and a smoother journey through what can often be a stressful time.
Knowing that multiple highly skilled professionals are cross-referencing information and working together seamlessly, often aided by advanced technology, gives you the confidence that you’re receiving the best possible care.
Q: What role does technology, particularly
A: I, play in strengthening this partnership, and what does the future hold for this collaboration? A3: Oh, this is where it gets really exciting! Technology, especially artificial intelligence, is truly a game-changer, acting as the ultimate bridge between medical technologists and radiographers.
Historically, lab data and imaging data often existed in “silos,” meaning they were stored and analyzed separately. But now, with advancements like digital imaging, robust data management systems, and cloud-based platforms, these two fields are converging.
AI is revolutionizing both disciplines. In radiology, AI algorithms are becoming incredibly adept at detecting subtle patterns in images that even the sharpest human eye might miss, helping identify early cancers or fractures with greater accuracy.
For medical technologists, AI can automate routine tasks, analyze vast datasets from patient samples, and uncover insights into disease progression that might not be apparent otherwise, leading to enhanced diagnostic precision.
The future of this collaboration, powered by AI and advanced IT, is heading towards “integrated diagnostics.” Imagine a system where your genomic data, lab results, and every medical image are seamlessly combined and analyzed by AI, providing an unbelievably comprehensive and predictive view of your health.
This integration promises earlier disease detection, highly personalized treatment strategies, and a massive leap in diagnostic efficiency. We’re looking at a future where AI not only supports these professionals but also empowers them to collaborate at an unprecedented level, leading to healthcare that’s smarter, faster, and truly patient-centric.
It’s an incredible time to be witnessing this evolution!